Weighing the Options: Bariatric Surgery vs. Weight Loss Drugs
Author

Beth Anderson, PA-C
Obesity has reached epidemic proportions in the U.S., and according to a Cleveland Clinic study, is now the leading cause of preventable death – topping tobacco use, diabetes, and high blood pressure.
More than two-thirds of Americans are overweight, which can lead to a lower quality of life and serious obesity-related medical conditions including diabetes, heart disease, high blood pressure, fatty liver disease, and sleep apnea.
Bariatric surgery has become a trusted, effective method for both weight loss and remission of some of these obesity-related diseases.
But the introduction of new prescription medications, such as Ozempic, Mounjaro, and Wegovy has many people questioning whether surgery or weight loss drugs is the best intervention for their obesity.
Here are six things to consider before deciding which weight loss option is right for you.
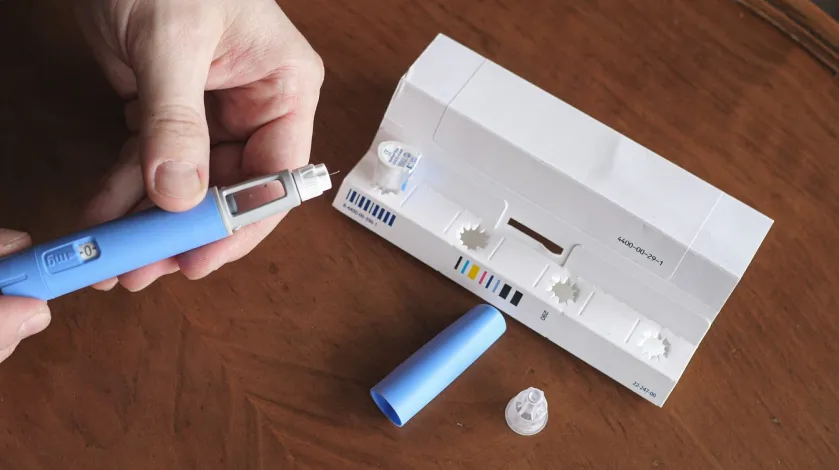
How do weight loss drugs like Ozempic and Wegovy work?
Known as Glucagon-like peptide-1 receptor agonists or GLP-1 agonists, Wegovy, Ozempic, and Mounjaro are injectable prescription medications typically administered once weekly.
Initially developed and approved for the treatment of type 2 diabetes, the GLP-1 Agonists have a side effect of substantial weight loss.
The medications work by mimicking the action of a gut hormone – GLP-1 – released after eating. This slows the movement of food in your gut, making you feel full longer, and works for weight loss by suppressing your appetite, so you crave and eat less food.
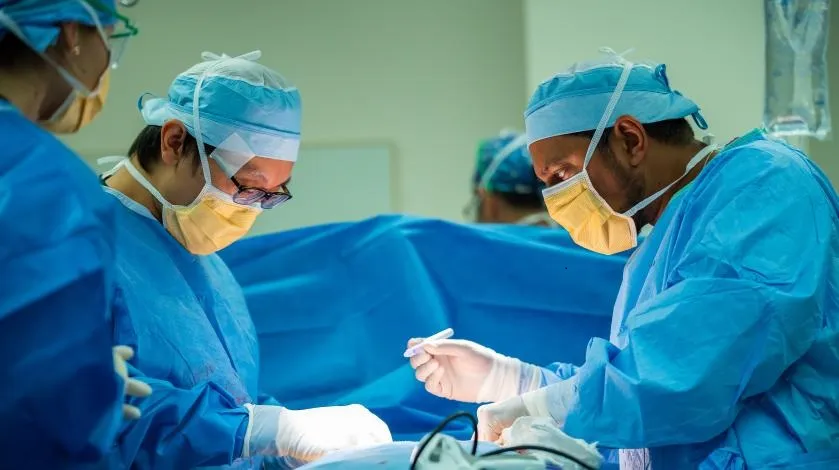
How does bariatric surgery work?
Bariatric surgery is effective for weight loss and has a metabolic effect that helps improve hunger, diabetes, and other obesity-related conditions.
Bariatric surgery works by decreasing the size of your stomach and, in some procedures, altering the digestive process and regulating how many calories you can consume and absorb.
It also reduces the hunger signals that travel from your digestive system to your brain and changes your metabolism.
When it comes to weight loss, how do bariatric surgery and medications compare?
Depending on the procedure performed, bariatric surgery patients lose an average of 25% to 35% of their body weight and 50% to 70% of their excess weight.
GLP-1 agonists are associated with about 15% to 20% of total body weight loss.
Recent studies favor bariatric surgery for overall weight loss and Body Mass Index (BMI) reduction, but show that both surgery and GLP-1 agonists have a similar effect for improvement in diabetes.
In addition to more significant weight loss and lower BMI, bariatric surgery has been shown to reduce the risk of death from any cause by more than 40%. It also lowers the risk of death by heart disease by 40%, cancer by 60%, and diabetes by 92%.
What are the barriers to bariatric surgery?
Current insurance qualifications for bariatric surgery are a BMI of 40 or greater or a BMI of 35 or greater along with obesity related co-morbidities such as diabetes, high blood pressure, or sleep apnea.
These recommendations go back 30 years and are considered outdated by many within the medical community.
In fact, it’s estimated that only 1% of all patients who would benefit from bariatric surgery would actually qualify for it based on these recommendations.
The American Society of Metabolic and Bariatric Surgery (ASMBS) recently released new recommendations for bariatric surgery that lower the BMI requirements to greater than 35 without co-morbidities and greater than 30 with co-morbidities.
We are working hard to lobby insurance companies to adopt these new recommendations, as we think patients would benefit from these updated guidelines.
What are the barriers to GLP-1 agonists?
The Federal Drug Administration (FDA) has approved Wegovy for the treatment of obesity and will likely approve more of the GLP-1 agonists for this use soon.
However, insurance carriers have not begun approving use of these medications for obesity alone; they are approved as treatment for type 2 diabetes.
Without insurance coverage, GLP-1 agonists come with a considerable cost – between $800 and $1,200 per month. The fact that the medication is taken as a weekly injection can be another obstacle for some patients.
Like other medications, GLP-1 agonists can cause side effects – the most common are nausea, vomiting and diarrhea, dizziness, mild rapid heart rate, infections, headaches, and heartburn.
And while these medications are effective for weight loss, patients do experience weight regain when they stop using them.
When would both surgery and GLP-1 agonists be the recommended treatment?
There are a few reasons we might recommend both GLP-1 agonists and surgery for obesity.
Patients with a weight of more than 500 lbs. will often benefit from medical management of their obesity prior to surgery. Risks of surgery are decreased when the BMI is closer to 50.
Weight regain is also a reality for some people after bariatric surgery. It is estimated that about one-fifth of patients regain more than 15% of their body weight five years after the procedure.
Reasons that patients regain weight post-surgery can include hormone re-regulation reducing the suppression of the “hunger hormone,” not adhering to diet, physical inactivity, and returning to pre-surgery habits.
To help reduce the risk of weight regain, we are now offering referral to our medical weight loss group for consideration of GLP-1 agonists.
How patients embark on their weight loss journey is a personal decision. Bariatric surgery and GLP-1 agonists are just two tools to use as a part of a lifestyle change supporting an overall improvement in health and quality of life.
Patients can get more information about weight loss options by attending one of our virtual information sessions and scheduling a consultation with our bariatric surgeon, Neil D. Ghushe, MD.
Beth Anderson, PA-C is the Program Manager at the South Shore Hospital Center for Metabolic and Bariatric Surgery. Learn more about weight loss surgery at South Shore Health.
Author

Beth Anderson, PA-C